TOPIC 10: Systems Physical Assessment I
Introduction:
The integumentary system, consisting of the skin, hair, and nails, is the largest organ of the body and the easiest of all systems to assess. The skin, hair, and nails provide clues about general health, reflect changes in environment, and signal internal ailments stemming from other organs. Therefore, a thorough assessment of this system may help you detect actual or potential problems, not only in the skin but also in underlying systems.
The head, face, and neck form a large portion of what is often referred to as the skull, face, eyes, ears, nose, sinuses, mouth, and pharynx. These components are complex in their actions and are involved in expression, communication, nourishment, respiration, and sensation, among other functions.
Topic Learning Outcome (TLOs):
By the end of this topic, you should be able to:
- Demonstrate an integumentary physical assessment.
- Document integumentary findings.
- Demonstrate a physical assessment of the skull, face, eyes, ears, nose, sinuses, mouth, and pharynx.
- Document skull, face, eyes, ears, nose, sinuses, mouth, and pharynx findings.
Structures and Functions of the Integumentary System

The structures of the integumentary system are the skin, hair, nails, sweat glands, and sebaceous glands. Their functions are described in the following table.

Performing an Integumentary Physical Assessment
Skin
Assessment of the skin involves inspection and palpation. The entire skin surface may be assessed at one time or as each aspect of the body is assessed. In some instances, the nurse may also use the olfactory sense to detect unusual skin odors; these are usually most evident in the skinfolds or in the axillae. Pungent body odor is frequently related to poor hygiene, hyperhidrosis (excessive perspiration), or bromhidrosis (foul-smelling perspiration).
Pallor is the result of inadequate circulating blood or haemoglobin and subsequent reduction in tissue oxygenation. In clients with dark skin, it is usually characterized by the absence of underlying red tones in the skin and may be most readily seen in the buccal mucosa. In brown-skinned clients, pallor may appear as a yellowish-brown tinge; in black-skinned clients, the skin may appear ashen gray. Pallor in all people is usually most evident in areas with the least pigmentation such as the conjunctiva, oral mucous membranes, nail beds, palms of the hand, and soles of the feet.Cyanosis (a bluish tinge) is most evident in the nail beds, lips, and buccal mucosa. In dark-skinned clients, close inspection of the palpebral conjunctiva (the lining of the eyelids) and palms and soles may also show evidence of cyanosis. Jaundice (a yellowish tinge) may first be evident in the sclera of the eyes and then in the mucous membranes and the skin. Nurses should take care not to confuse jaundice with the normal yellow pigmentation in the sclera of a dark-skinned client. If jaundice is suspected, the posterior part of the hard palate should also be inspected for a yellowish color tone. Erythema is skin redness associated with a variety of rashes and other conditions.
Localized areas of hyperpigmentation (increased pigmentation) and hypopigmentation (decreased pigmentation) may occur as a result of changes in the distribution of melanin (the dark pigment) or in the function of the melanocytes in the epidermis. An example of hyperpigmentation in a defined area is a birthmark; an example of hypopigmentation is vitiligo. Vitiligo, seen as patches of hypopigmented skin, is caused by the destruction of melanocytes in the area. Albinism is the complete or partial lack of melanin in the skin, hair, and eyes. Other localized color changes may indicate a problem such as edema or a localized infection. Dark-skinned clients normally have areas of lighter pigmentation, such as the palms, lips, and nail beds.
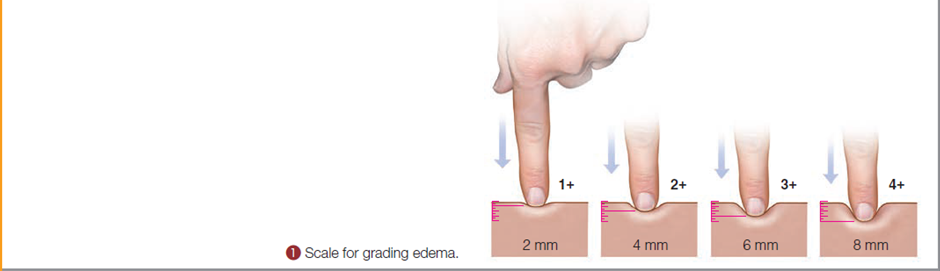
Edema is the presence of excess interstitial fluid. An area of edema appears swollen, shiny, and taut and tends to blanch the skin color or, if accompanied by inflammation, may redden the skin. Generalized edema is most often an indication of impaired venous circulation and in some cases reflects cardiac dysfunction or venous abnormalities.
A skin lesion is an alteration in a client’s normal skin appearance. Primary skin lesions are those that appear initially in response to some change in the external or internal environment of the skin as in table below.

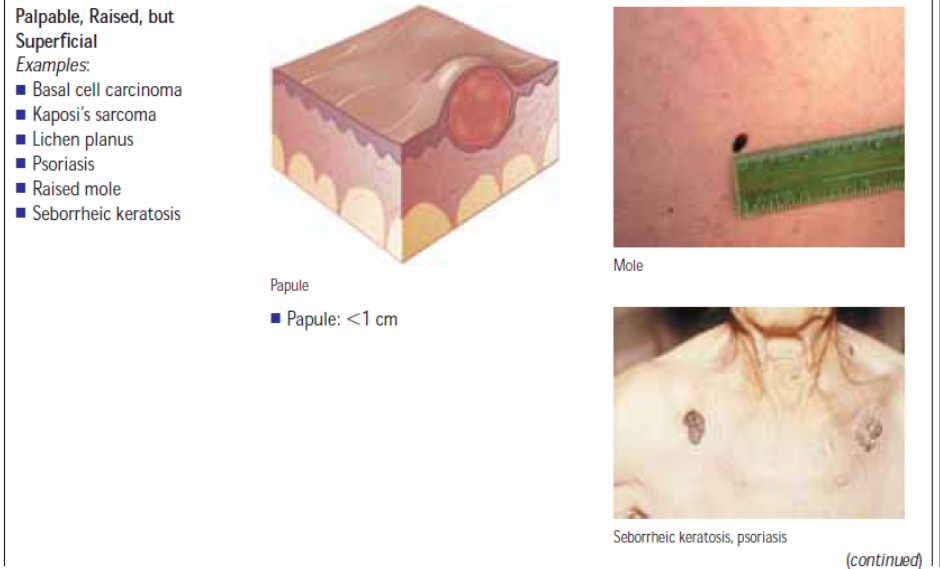

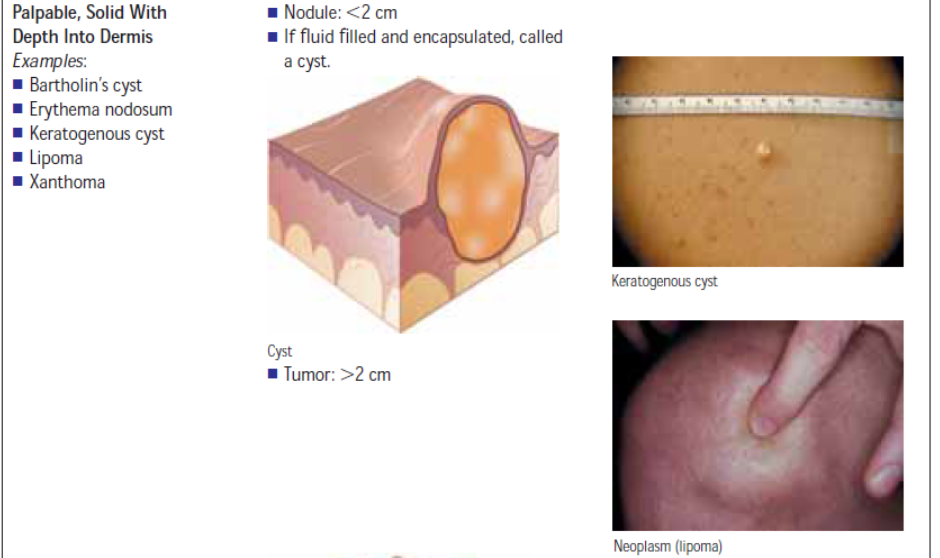

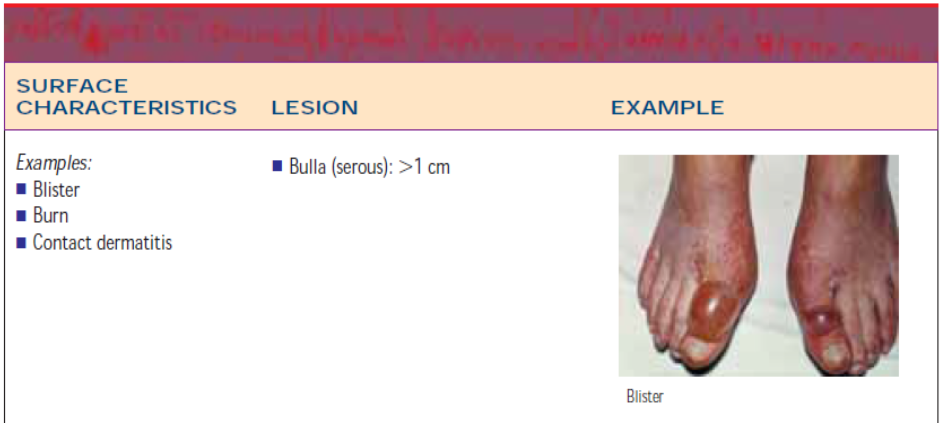
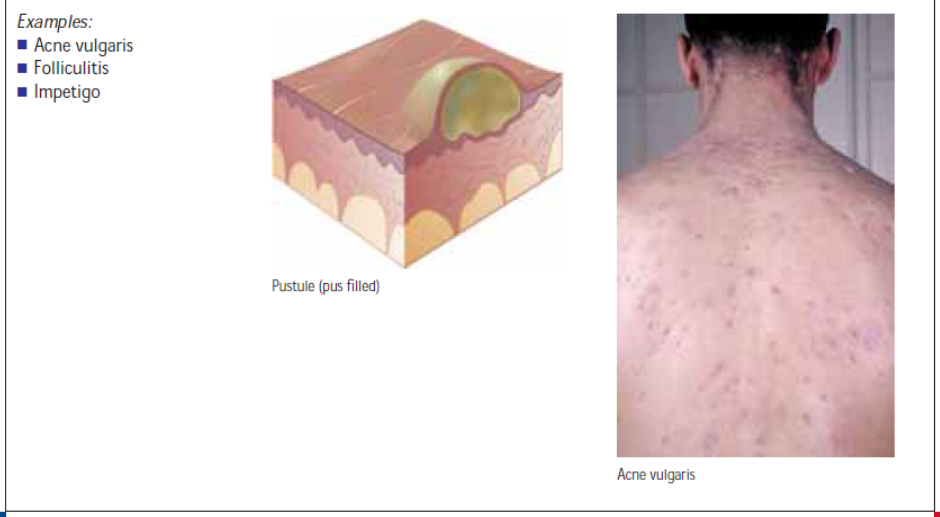
Secondary skin lesions are those that do not appear initially but result from modifications such as chronicity, trauma, or infection of the primary lesion. For example, a vesicle or blister (primary lesion) may rupture and cause an erosion (secondary lesion). Table below illustrates secondary lesions.


Nurses are responsible for describing skin lesions accurately in terms of location (e.g., face), distribution (i.e., body regions involved), and configuration (the arrangement or position of several lesions) as well as color, shape, size, firmness, texture, and characteristics of individual lesions. The following table describes how to assess the skin.





Hair
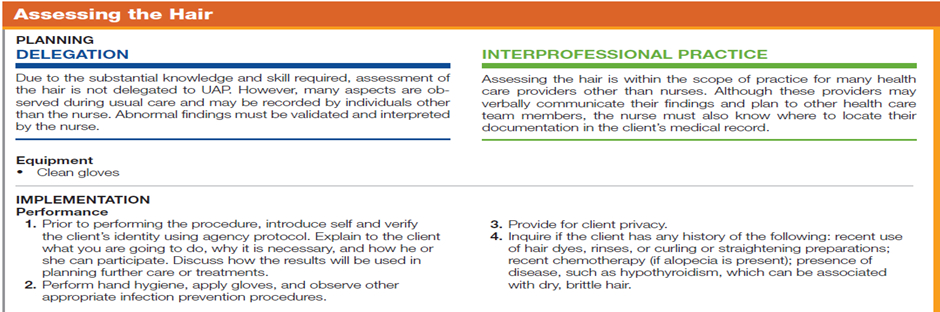
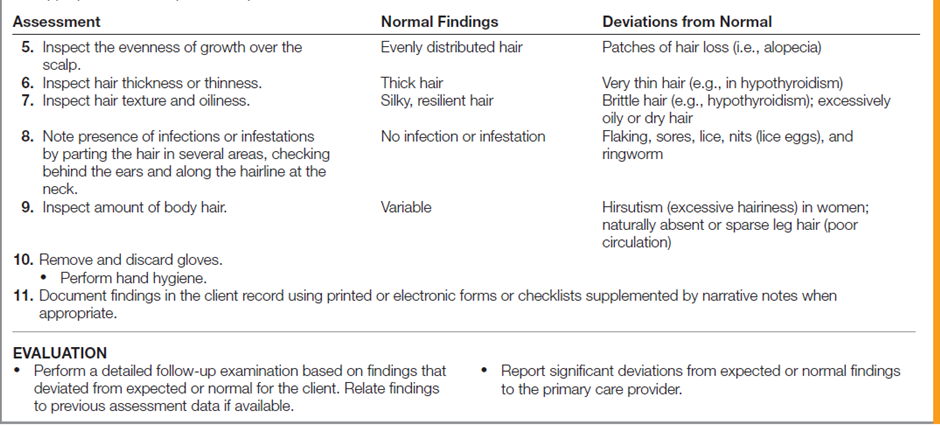
Assessing a client’s hair includes inspecting the hair, considering developmental changes and ethnic differences, and determining the individual’s hair care practices and factors influencing them. Much of the information about hair can be obtained by questioning the client.
Normal hair is resilient and evenly distributed. In people with severe protein deficiency (kwashiorkor), the hair color is faded and appears reddish or bleached, and the texture is coarse and dry. Some therapies cause alopecia (hair loss), and some disease conditions and medications affect the coarseness of hair. For example, hypothyroidism can cause very thin and brittle hair. The table below describes how to assess the hair.

Nails
Nails are inspected for nail plate shape, angle between the fingernail and the nail bed, nail texture, nail bed color, and the intactness of the tissues around the nails. The parts of the nail are shown in Figure below.
The nail plate is normally colorless and has a convex curve. The angle between the fingernail and the nail bed is normally 160 degrees. One nail abnormality is the spoon shape, in which the nail curves upward from the nail bed. This condition, called koilonychia, may be seen in clients with iron deficiency anemia. Clubbing is a condition in which the angle between the nail and the nail bed is 180 degrees, or greater. Clubbing may be caused by a long-term lack of oxygen.
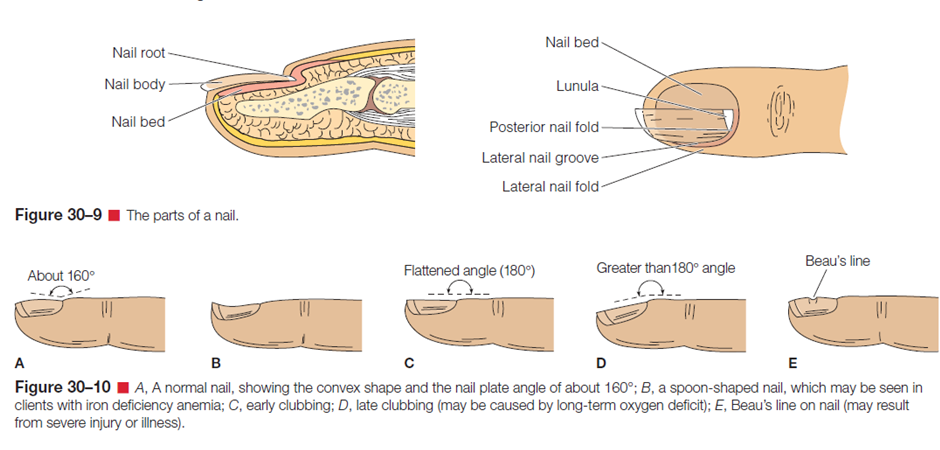
Nail texture is normally smooth. Excessively thick nails can appear in older adults, in the presence of poor circulation, or in relation to a chronic fungal infection. Excessively thin nails or the presence of grooves or furrows can reflect prolonged iron deficiency anemia. Beau’s lines are horizontal depressions in the nail that can result from injury or severe illness. The nail bed is highly vascular, a characteristic that accounts for its color. A bluish or purplish tint to the nail bed may reflect cyanosis, and pallor may reflect poor arterial circulation. Should the client report a history of nail fungus (onychomycosis), a referral to a podiatrist or dermatologist for treatment of nail fungus may be appropriate. Symptoms of nail fungus includes brittleness, discoloration, thickening, distortion of nail shape, crumbling of the nail, and loosening (detaching) of the nail.
The tissue surrounding the nails is normally intact epidermis. Paronychia is an inflammation of the tissues surrounding a nail. The tissues appear inflamed and swollen, and tenderness is usually present.
A blanch test can be carried out to test the capillary refill, that is, peripheral circulation. Normal nail bed capillaries blanch when pressed, but quickly turn pink or their usual color when pressure is released. A slow rate of capillary refill may indicate circulatory problems.
The table below describes how to assess the nails.


Documentation
Skin is expected color for ethnicity without lesions or rashes. Skin is warm and dry with no
edema. Capillary refill is less than 3 seconds. Normal skin turgor with no tenting.
For better understanding and practice, you may watch the following videoclip on “Physical Examination of the Skin”
Video:HEAD
During assessment of the head, the nurse inspects and palpates simultaneously and also auscultates. The nurse examines the skull, face, eyes, ears, nose, sinuses, mouth, and pharynx.
Structures of the Skull and Face
Skull and Face
There is a large range of normal shapes of skulls. A normal head size is referred to as normocephalic. If head size appears to be outside of the normal range, the circumference can be compared to standard size tables. Measurements more than two standard deviations from the norm for the age, sex, and race of the client are abnormal and should be reported to the primary care provider. Names of areas of the head are derived from names of the underlying bones: frontal, parietal, occipital, mastoid process, mandible, maxilla, and zygomatic. The following diagram shown the structure of skull and face.

Many disorders cause a change in facial shape or condition. Kidney or cardiac disease can cause edema of the eyelids. Hyperthyroidism can cause exophthalmos, a protrusion of the eyeballs with elevation of the upper eyelids, resulting in a startled or staring expression. Hypothyroidism, or myxedema, can cause a dry, puffy face with dry skin and coarse features and thinning of scalp hair and eyebrows.
Increased adrenal hormone production or administration of steroids can cause a round face with reddened cheeks, referred to as moon face, and excessive hair growth on the upper lips, chin, and sideburn areas. Prolonged illness, starvation, and dehydration can result in sunken eyes, cheeks, and temples.
Performing The Skull and Face Physical Assessment
Table below describes how to assess the skull and face.


Documentation
Skull
§ Generally round, with prominences in the frontal and occipital area. (Normocephalic).
§ No tenderness noted upon palpation.Scalp
§ Lighter in color than the complexion.
§ Can be moist or oily.
§ No scars noted.
§ Free from lice, nits and dandruff.
§ No lesions should be noted.
§ No tenderness or masses on palpation.Hair
§ Can be black, brown or burgundy depending on the race.
§ Evenly distributed covers the whole scalp (No evidences of Alopecia)
§ Maybe thick or thin, coarse or smooth.
§ Neither brittle nor dry.Face
§ Shape maybe oval or rounded.
§ Face is symmetrical.
§ No involuntary muscle movements.
§ Can move facial muscles at will.
§ Intact cranial nerve V and VII.Structures of the Eyes
Eyes
Examination of the eyes includes assessment of the external structures, visual acuity (the degree of detail the eye can discern in an image), ocular movement, and visual fields (the area an individual can see when looking straight ahead). Most eye assessment procedures involve inspection. Consideration is also given to developmental changes and to individual hygienic practices, if the client wears contact lenses or has an artificial eye. For the anatomic structures of the eye, see the below diagram.

Many people wear eyeglasses or contact lenses to correct common refractive errors of the lens of the eye. These errors include myopia (nearsightedness), hyperopia (farsightedness), and presbyopia (loss of elasticity of the lens and thus loss of ability to see close objects). Presbyopia begins at about 45 years of age. People notice that they have difficulty reading newsprint. When both far and near vision require correction, two lenses (bifocals) are required. Astigmatism, an uneven curvature of the cornea that prevents horizontal and vertical rays from focusing on the retina, is a common problem that may occur in conjunction with myopia and hyperopia. Astigmatism may be corrected with glasses or surgery.
Common inflammatory visual problems that nurses may encounter in clients include conjunctivitis, dacryocystitis, hordeolum, iritis, and contusions or hematomas of the eyelids and surrounding structures. Conjunctivitis (inflammation of the bulbar and palpebral conjunctiva) may result from foreign bodies, chemicals, allergenic agents, bacteria, or viruses. Redness, itching, tearing, and mucopurulent discharge occurs. During sleep, the eyelids may become encrusted and matted together. Dacryocystitis (inflammation of the lacrimal sac) is manifested by tearing and a discharge from the nasolacrimal duct. Hordeolum (sty) is a redness, swelling, and tenderness of the hair follicle and glands that empty at the edge of the eyelids. Iritis (inflammation of the iris) may be caused by local or systemic infections and results in pain, tearing, and photophobia (sensitivity to light). Contusions or hematomas are “black eyes” resulting from injury.
Cataracts tend to occur in individuals over 65 years old although they may be present at any age. This opacity of the lens or its capsule, which blocks light rays, is frequently removed and replaced by a lens implant. Cataracts may also occur in infants due to a malformation of the lens if the mother contracted rubella in the first trimester of pregnancy. Glaucoma (a disturbance in the circulation of aqueous fluid, which causes an increase in intraocular pressure) is the most frequent cause of blindness in people over age 40 although it can occur at younger ages. It can be controlled if diagnosed early. Danger signs of glaucoma include blurred or foggy vision, loss of peripheral vision, difficulty focusing on close objects, difficulty adjusting to dark rooms, and seeing rainbow-colored rings around lights.
Upper eyelids that lie at or below the pupil margin are referred to as ptosis and are usually associated with aging, edema from drug allergy or systemic disease (e.g., kidney disease), congenital lid muscle dysfunction, neuromuscular disease (e.g., myasthenia gravis), and third cranial nerve impairment. Eversion, an outturning of the eyelid, is called ectropion; inversion, an inturning of the lid, is called entropion. These abnormalities are often associated with scarring injuries or the aging process.
Pupils are normally black, are equal in size (about 3 to 7 mm in diameter), and have round, smooth borders. Cloudy pupils are often indicative of cataracts. Mydriasis (enlarged pupils) may indicate injury or glaucoma, or result from certain drugs (e.g., atropine, cocaine, amphetamines). Miosis (constricted pupils) may indicate an inflammation of the iris or result from such drugs as morphine/heroin and other narcotics, barbiturates, or pilocarpine. It is also an age-related change in older adults. Anisocoria (unequal pupils) may result from a central nervous system disorder; however, slight variations may be normal. The iris is normally flat and round. A bulging toward the cornea can indicate increased intraocular pressure.
Performing Eyes Physical Assessment
The following table describes how to assess a client’s eye structures and visual acuity.
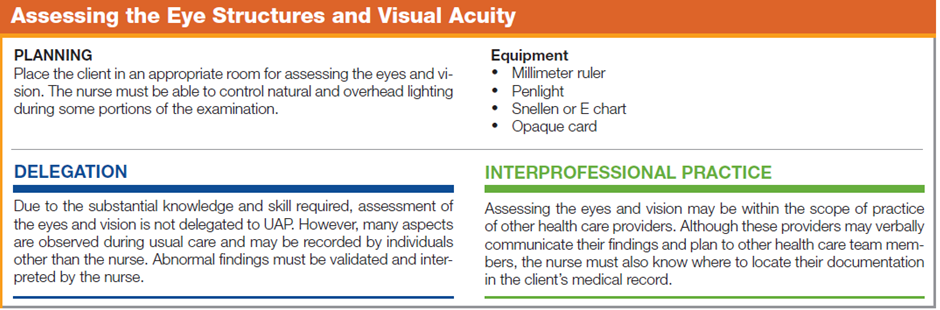
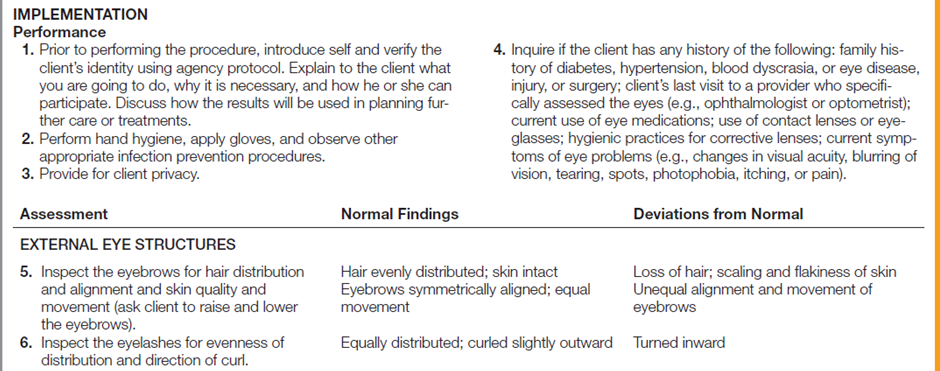



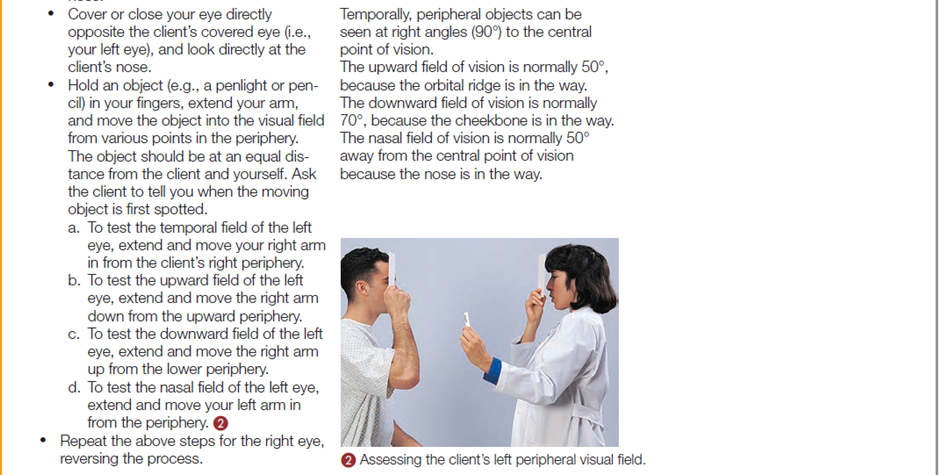

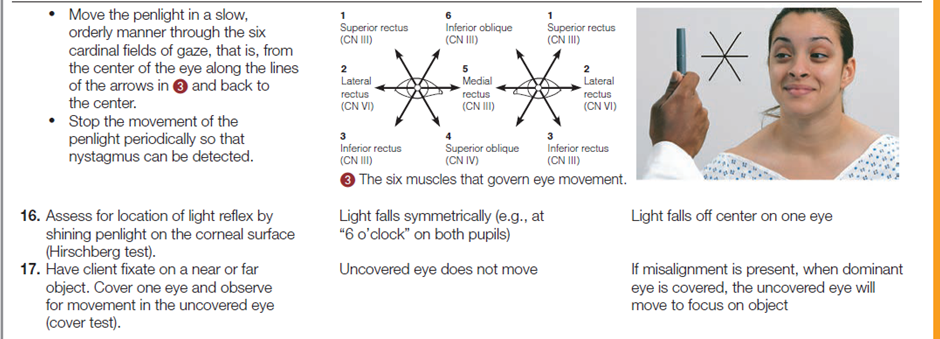



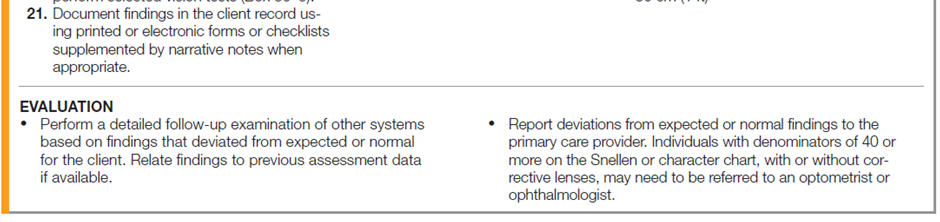
Documentation
Eyebrows
§ Symmetrical and in line with each other.
§ Maybe black, brown or blond depending on race.
§ Evenly distributed.Eyes
§ Evenly placed and in line with each other.
§ None protruding.
§ Equal palpebral fissure.Eyelashes
§ Color dependent on race.
§ Evenly distributed.
§ Turned outward.Eyelids
§ Upper eyelids cover the small portion of the iris, cornea, and sclera when eyes are open.
§ No PTOSIS noted. (Drooping of upper eyelids).
§ Meets completely when eyes are closed.
§ Symmetrical.Lacrimal Apparatus
§ Lacrimal gland is normally non-palpable.
§ No tenderness on palpation.
§ No regurgitation from the nasolacrimal duct.Conjunctivae
§ Both conjunctivae are pinkish or red in color.
§ With presence of many minutes capillaries.
§ Moist
§ No ulcers
§ No foreign objectsSclerae
§ Sclerae is white in color (anicteric sclera)
§ No yellowish discoloration (icteric sclera).
§ Some capillaries maybe visible.
§ Some people may have pigmented positions.Cornea
§ There should be no irregularities on the surface.
§ Looks smooth.
§ The cornea is clear or transparent. The features of the iris should be fully visible through the cornea.
§ There is a positive corneal reflex.Anterior Chamber and Iris
§ The anterior chamber is transparent.
§ No noted any visible materials.
§ Color of the iris depends on the person’s race (black, blue, brown or green).
§ From the side view, the iris should appear flat and should not be bulging forward. There should be NO crescent shadow casted on the other side when illuminated from one side.Pupils
§ Pupillary size ranges from 3 – 7 mm, and are equal in size.
§ Equally round.
§ Constrict briskly/sluggishly when light is directed to the eye, both directly and consensual.
§ Pupils dilate when looking at distant objects, and constrict when looking at nearer objects.
§ If all of which are met, we document the findings using the notation PERRLA, pupils equally round, reactive to light, and accommodateVisual Acuity (Cranial Nerve II – Optic Nerve)
§ The normal vision at a set distance at 20/20.
§ Peripheral Vision or visual fields - The normal visual field is 180 degrees.Cranial Nerve III, IV & VI (Oculomotor, Trochlear, Abducens)
§ The client can hold the position and there should be no nystagmus.
Structures of the Ears
Ears
Assessment of the ear includes direct inspection and palpation of the external ear, inspection of the internal parts of the ear by an otoscope (instrument for examining the interior of the ear, especially the eardrum, consisting essentially of a magnifying lens and a light), and determination of auditory acuity.
The ear is divided into three parts: external ear, middle ear, and inner ear. Many of the structures discussed next are illustrated in diagram below.
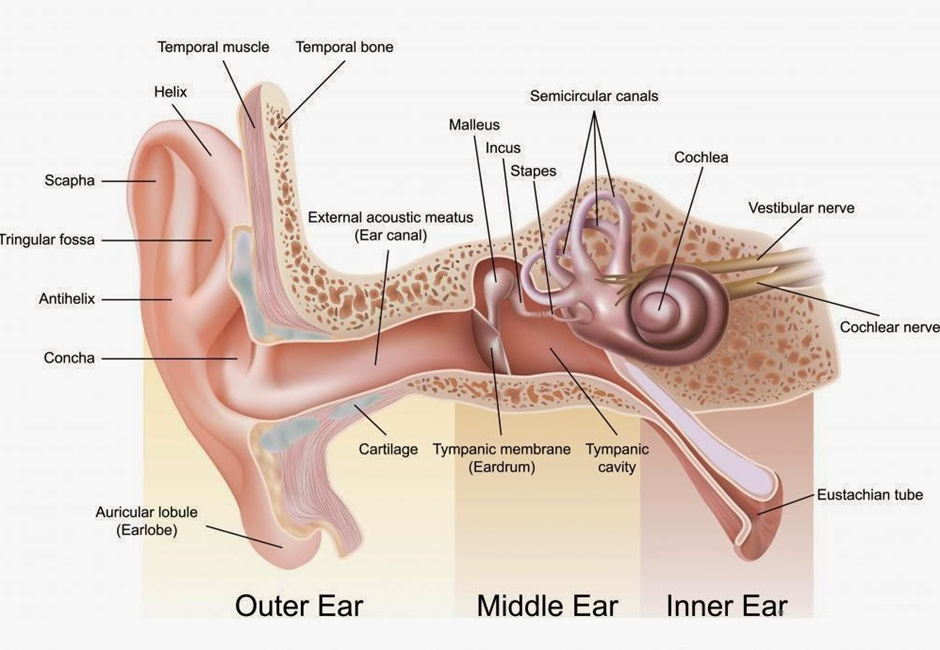
Sound transmission and hearing are complex processes. In brief, sound can be transmitted by air conduction or bone conduction. Air conducted transmission occurs by this process:
1. A sound stimulus enters the external canal and reaches the tympanic membrane.
2. The sound waves vibrate the tympanic membrane and reach the ossicles.
3. The sound waves travel from the ossicles to the opening in the inner ear (oval window).
4. The cochlea receives the sound vibrations.
5. The stimulus travels to the auditory nerve (the eighth cranial nerve) and the cerebral cortex.
Bone-conducted sound transmission occurs when skull bones transport the sound directly to the auditory nerve. Conductive hearing loss is the result of interrupted transmission of sound waves through the outer and middle ear structures. Possible causes are a tear in the tympanic membrane or an obstruction, due to swelling or other causes, in the auditory canal. Sensorineural hearing loss is the result of damage to the inner ear, the auditory nerve, or the hearing center in the brain. Mixed hearing loss is a combination of conduction and sensorineural loss.
Performing Ears Physical Assessment
The table below describes how to assess the ears and hearing.
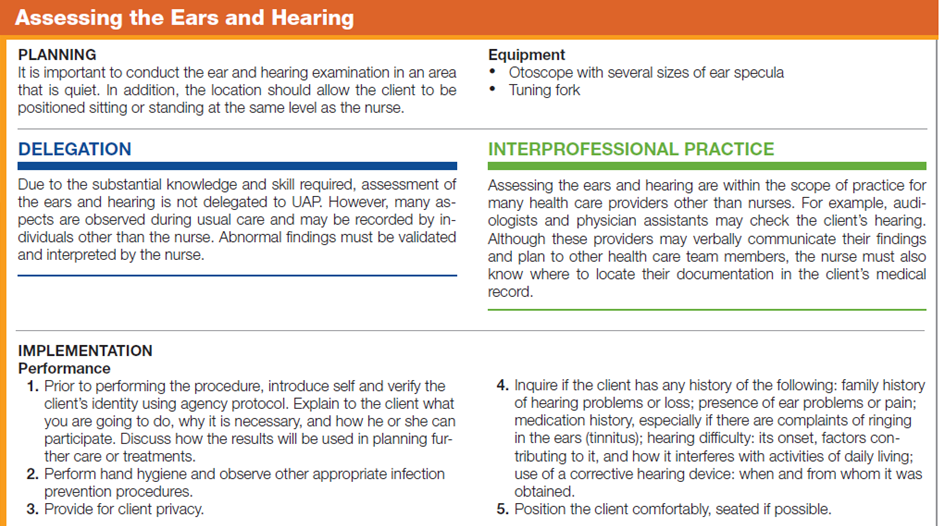

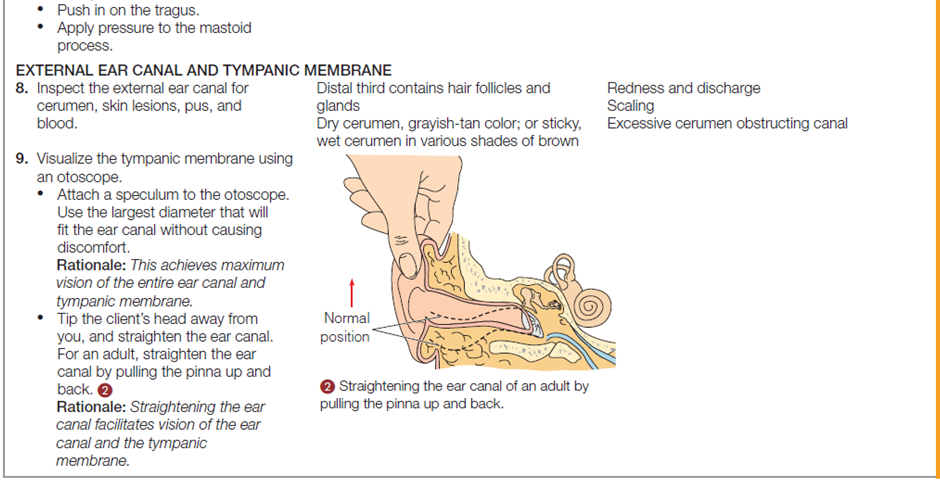
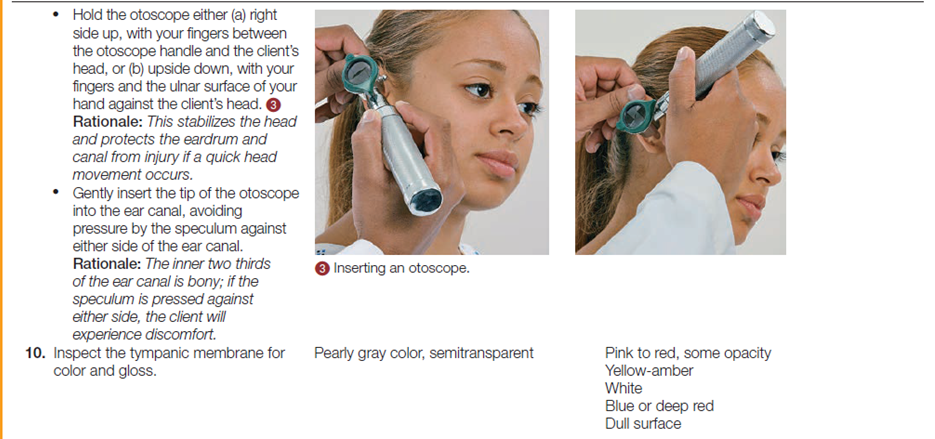


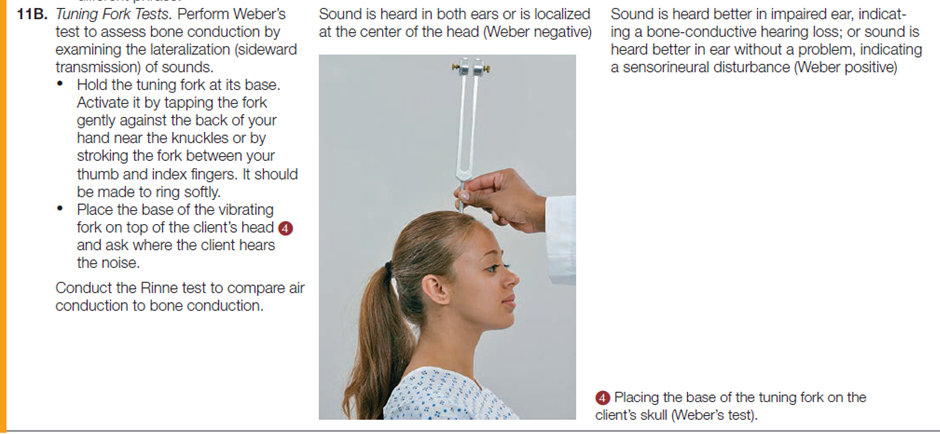

Documentation
§ The ear lobes are bean shaped, parallel, and symmetrical.
§ The upper connection of the ear lobe is parallel with the outer canthus of the eye.
§ Skin is same in color as in the complexion.
§ No lesions noted on inspection.
§ The auricles are have a firm cartilage on palpation.
§ The pinna recoils when folded.
§ There is no pain or tenderness on the palpation of the auricles and mastoid process.
§ The ear canal has normally some cerumen of inspection.
§ No discharges or lesions noted at the ear canal.
§ On otoscopic examination the tympanic membrane appears flat, translucent and pearly gray in color.For better understanding and practice, you may watch the following videoclip on “Physical Examination of the Head, Eyes and”
Video: https://youtu.be/O1MnyQMy6dI?list=PLBdcS7ILKLhRP4w0R6CjLXpWC4-BX_ABv&t=446
Nose and Sinuses
Structures and Functions of the Nose and Sinuses
A nurse can inspect the nasal passages very simply with a flashlight. However, a nasal speculum and a penlight or an otoscope with a nasal attachment facilitates examination of the nasal cavity. Assessment of the nose includes inspection and palpation of the external nose (the upper third of the nose is bone; the remainder is cartilage); patency of the nasal cavities; and inspection of the nasal cavities.
If the client reports difficulty or abnormality in smell, the nurse may test the client’s olfactory sense by asking the client to identify common odors such as coffee or mint. This is done by asking the client to close the eyes and placing vials containing the scent under the client’s nose. The nurse also inspects and palpates the facial sinuses as in the diagram below.
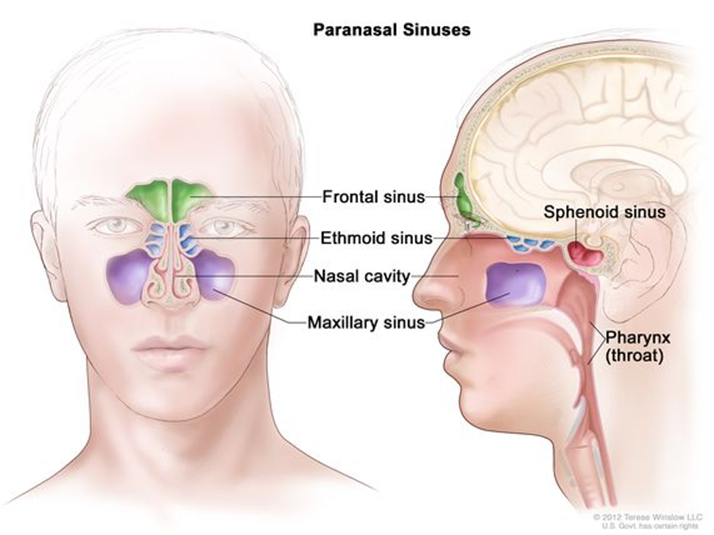
Performing the Nose and Sinuses Physical Assessment
The table below describes how to assess the nose and sinuses.
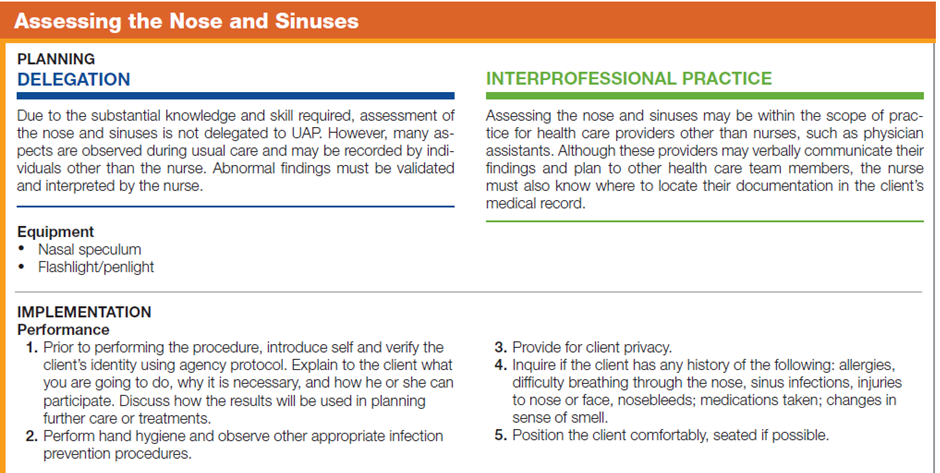

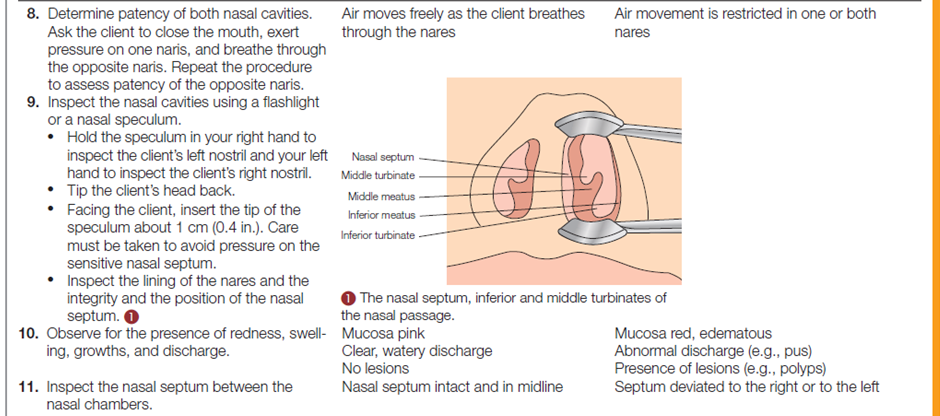

Documentation
§ Nose in the midline
§ No Discharges.
§ No flaring alae nasi.
§ Both nares are patent.
§ No bone and cartilage deviation noted on palpation.
§ No tenderness noted on palpation.
§ Nasal septum in the mid line and not perforated.
§ The nasal mucosa is pinkish to red in color. (Increased redness turbinates are typical of allergy).
§ No tenderness noted on palpation of the paranasal sinuses.
§ Cranial Nerve I (Olfactory Nerve) – The client was able to differentiate two given substances.Mouth and Oropharynx
Structures and Functions of the Mouth and Oropharynx
The mouth and oropharynx are composed of a number of structures: lips, oral mucosa, the tongue and floor of the mouth, teeth and gums, hard and soft palate, uvula, salivary glands, tonsillar pillars, and tonsils. Anatomic structures of the mouth are shown in diagram below.
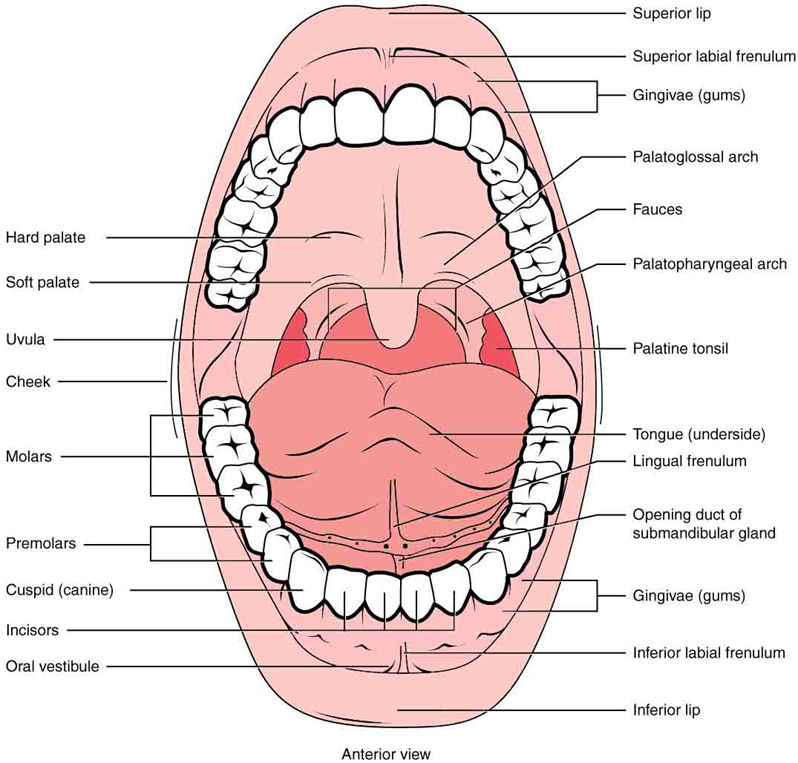
Normally, three pairs of salivary glands empty into the oral cavity: the parotid, submandibular, and sublingual glands. The parotid gland is the largest and empties through Stensen’s duct opposite the second molar. The submandibular gland empties through Wharton’s duct, which is situated on either side of the frenulum on the floor of the mouth. The sublingual salivary gland lies in the floor of the mouth and has numerous openings.
Dental caries (cavities) and periodontal disease (or pyorrhea) are the two problems that most frequently affect the teeth. Both problems are commonly associated with plaque and tartar deposits. Plaque is an invisible soft film that adheres to the enamel surface of teeth; it consists of bacteria, molecules of saliva, and remnants of epithelial cells and leukocytes. When plaque is unchecked, tartar (dental calculus) forms. Tartar is a visible, hard deposit of plaque and dead bacteria that forms at the gum lines. Tartar buildup can alter the fibers that attach the teeth to the gum and eventually disrupt bone tissue. Periodontal disease is characterized by gingivitis (red, swollen gingiva [gum]), bleeding, receding gum lines, and the formation of pockets between the teeth and gums. In advanced periodontal disease, the teeth are loose and pus is evident when the gums are pressed.
Other problems nurses may see are glossitis (inflammation of the tongue), stomatitis (inflammation of the oral mucosa), and parotitis (inflammation of the parotid salivary gland). The accumulation of foul matter (food, microorganisms, and epithelial elements) on the teeth and gums is referred to as sores.
Performing the Mouth and Oropharynx Physical AssessmentThe table below describes how to assess the mouth and oropharynx.





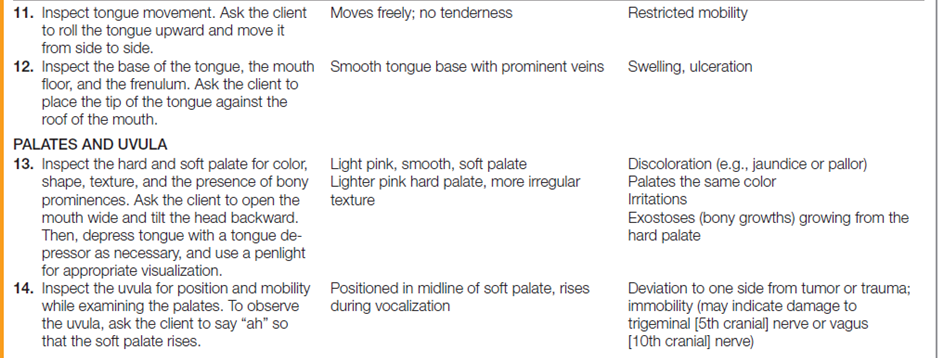

Documentation
Mouth and Oropharynx Lips
1. With visible margin
2. Symmetrical in appearance and movement
3. Pinkish in color
4. No edemaTemporomandibular
1. Moves smoothly no crepitous.
2. No deviations noted
3. No pain or tenderness on palpation and jaw movement.Gums
1. Pinkish in color
2. No gum bleeding
3. No receding gumsTeeth
1. 28 for children and 32 for adults.
2. White to yellowish in color
3. With or without dental carries and/or dental fillings.
4. With or without malocclusions.
5. No halitosis.Tongue
1. Pinkish with white taste buds on the surface.
2. No lesions noted.
3. No varicosities on ventral surface.
4. Frenulum is thin attaches to the posterior 1/3 of the ventral aspect of the tongue.
5. Gag reflex is present.
6. Able to move the tongue freely and with strength.
7. Surface of the tongue is rough.Uvula
1. Positioned in the mid line.
2. Pinkish to red in color.
3. No swelling or lesion noted.
4. Moves upward and backwards when asked to say “ah”Tonsils
1. No swelling or inflammation noted.
Neck
Structures and Functions of the Neck
Examination of the neck includes the muscles, lymph nodes, trachea, thyroid gland, carotid arteries, and jugular veins. Areas of the neck are defined by the sternocleidomastoid muscles, which divide each side of the neck into two triangles: the anterior and posterior as shown in the following diagram.
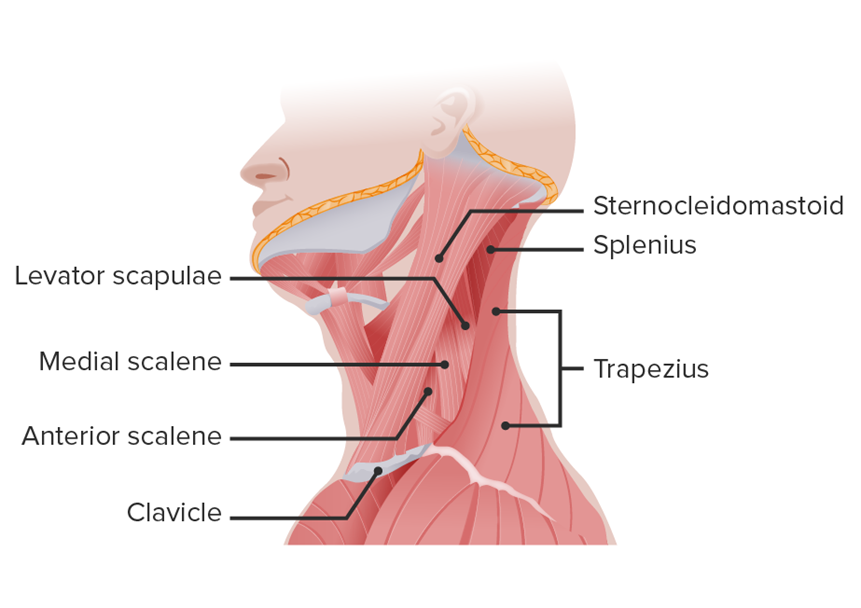
The trachea, thyroid gland, anterior cervical nodes, and carotid artery lie within the anterior triangle; the carotid artery runs parallel and anterior to the sternocleidomastoid muscle as shown in the following diagram.

Each sternocleidomastoid muscle extends from the upper sternum and the medial third of the clavicle to the mastoid process of the temporal bone behind the ear. These muscles turn and laterally flex the head. Each trapezius muscle extends from the occipital bone of the skull to the lateral third of the clavicle. These muscles draw the head to the side and back, elevate the chin, and elevate the shoulders to shrug them. The posterior lymph nodes lie within the posterior triangle as in the following diagram.
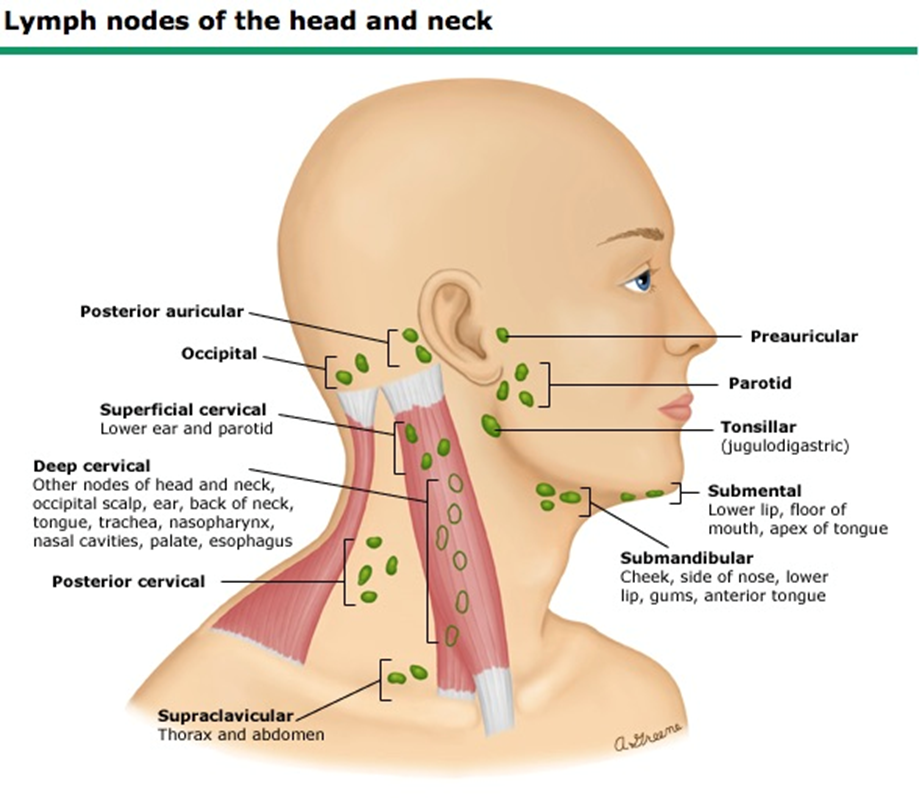
Lymph nodes in the neck that collect lymph from the head and neck structures are grouped serially and referred to as chains. Table below shown the lymph nodes and its location.
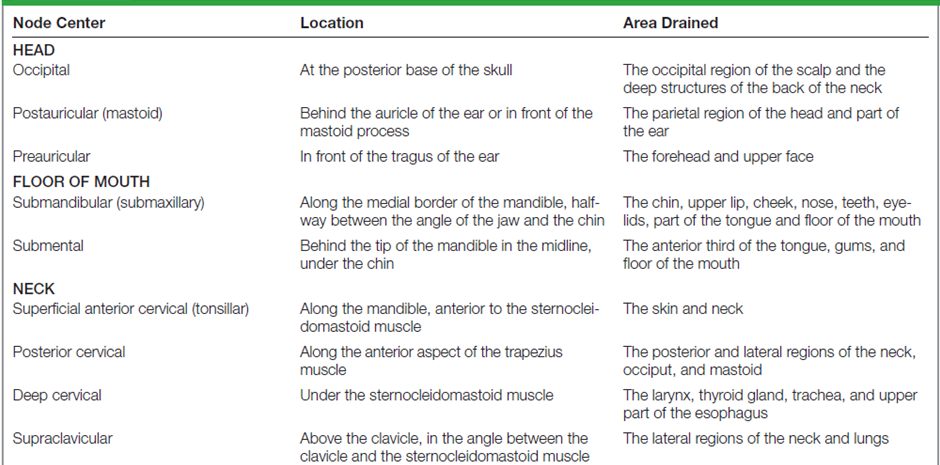
Performing the Neck Physical Assessment
The table below describes how to assess the neck.
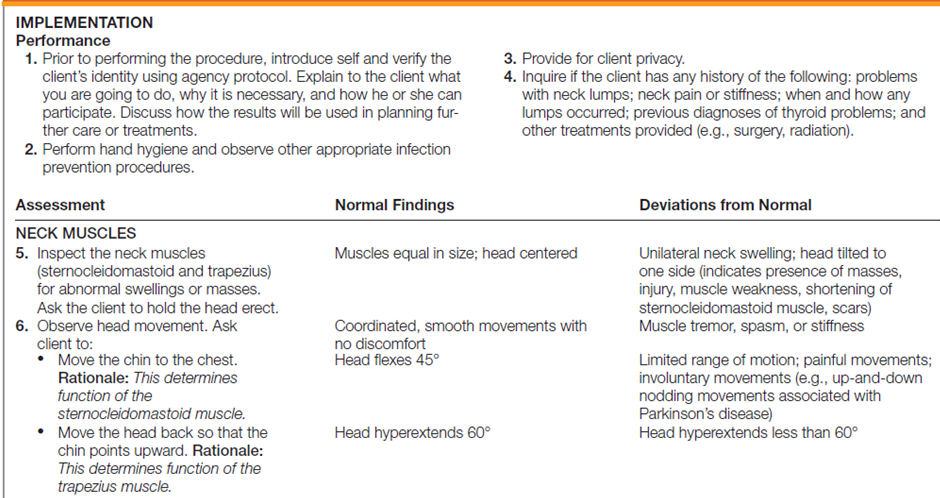



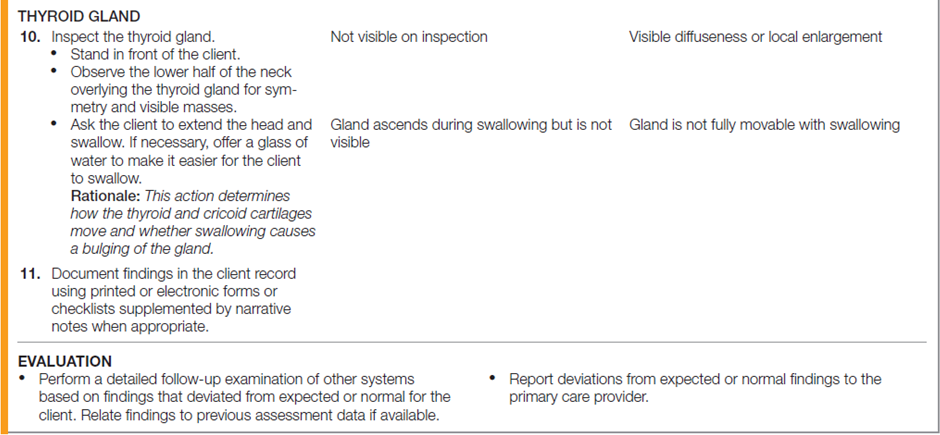
Documentation
Neck
§ Non-tender if palpable.
§ The neck is straight.
§ No visible mass or lumps.
§ Symmetrical
§ No jugular venous distension (suggestive of cardiac congestion).
§ The trachea is palpable - It is positioned in the line and straight.Lymph nodes
§ May not be palpable. Maybe normally palpable in thin clients.
§ Non-tender if palpable.
§ Firm with smooth rounded surface.
§ Slightly movable.
§ About less than 1 cm in size.Thyroid
§ Normally the thyroid is non-palpable.
§ Isthmus maybe visible in a thin neck.
§ No nodules are palpable.
§ No bruits sound heard on auscultation.For better understanding and practice, you may watch the following videoclip on “Physical Examination of the Nose, Mouth and Neck”
Video: